When lockdown first hit in March 2020, we were acutely aware of the number of Old Stoics working on the front line. We asked them to share their experiences so we could have the opportunity to thank them for everything they are doing.
 Emma Whiting (Stanhope 14)
Emma Whiting (Stanhope 14)
“As the first cases of Covid-19 started to grumble at the beginning of the year, I was a final year medical student preparing to take my final exams. I had a 3-month elective planned (a period working in Vanuatu, putting my new medical skills into practice and exploring the South Pacific) before starting work officially in August 2020. Little did I know that all these plans would be turned upside down.
I took my final exams in the weeks just before lockdown and my graduation and registration as a doctor were expedited to allow us to help with the Covid-19 crisis. Shortly afterwards, I was launched into my first job as a doctor in a busy London hospital that had been hit particularly hard by the pandemic. It was not what I imagined would happen at the end of my time at Medical School and I was terrified to enter the NHS at such a critical time.
It has been the steepest learning curve of my life, but has only made me more prepared and excited for work in the future. Even during the most hectic of days with the most unwell patients, there is always something to reflect on of which I am proud. It has been humbling to see an (already strained) NHS come together so fantastically – new skills have been learnt incredibly quickly; jobs have changed with little notice; working hours have increased and new doctors, along with those coming out of retirement, have jumped at the chance to help. Whatever their skillset, everybody has relished the opportunity to make a difference wherever possible. This is something that is very special indeed.
I am due to start a different job on a respiratory ward in August and I feel as prepared as I can possibly be. I’m sure there will be time to explore the South Pacific later in life!”
 Imy O’Brien (Nugent 13)
Imy O’Brien (Nugent 13)
”I normally work as a Musculoskeletal Physiotherapist in a GP practice in Fulham but I volunteered to redeploy to the Nightingale at the Excel where I led the proning team during my shifts. Proning – the technique of laying patients on their front – was incredibly important for the treatment of Covid-19 patients and was one of the more effective treatments that we had at our disposal.
It was quite the change from my everyday work, having never worked in an ICU setting, but along with the highs and lows it was an incredible experience. I have felt inspired by the other health care professionals I have met and feel privileged to have been able to play a small part.”
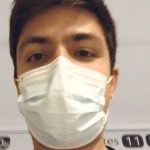 Matteo Di Carlofelice (Chatham 13)
Matteo Di Carlofelice (Chatham 13)
“After leaving Stowe in 2013 I completed my medical training at Imperial College School of Medicine in West London and have since moved to Leeds for my foundation training as a newly qualified doctor. The Covid-19 pandemic has certainly been a challenge during my first year of work.
It has been particularly difficult seeing usually independent people requiring breathing support and quickly deteriorating during my shifts. The ban on visitors has led to me and other junior colleagues frequently having to update family members over the phone, all too often with sad news. Lastly, increased out-of-hours work and adapting to rapidly evolving and unfamiliar environments has been tiring.
I have, however, had the opportunity to reflect on the positives. There has been a sense of camaraderie amongst the staff where I work as we come together during this time. Equally, it has been impressive to see those in leadership positions remaining dynamic in their response to government guidance and a PPE shortage. Finally, the support from the public has been amazing for all of us in a key worker position and we appreciate the sacrifices that everyone has made for the sake of protecting the NHS.”
 Lucie Wellington (Nugent 13)
Lucie Wellington (Nugent 13)
“I usually work within a team that focuses on the rehabilitation of elderly patients, with some weekends spent helping on the Intensive Care Unit (ICU). During the pandemic, I was redeployed to ICU full time, working as a respiratory physio. This included things such as optimising positioning, assisting with chest clearance, helping reduce ventilator support and post intensive care rehabilitation. It was mentally and physically exhausting but the support from the local community and beyond made coming into work to an unknown challenge every day a little easier.
I was so pleased to see the coming together of voices to praise those working in the NHS. I even found out one of my friends from Stowe, Imy O’Brien (Nugent 13), was working at the Nightingale Hospital after seeing a picture of her on Twitter being thanked by a colleague.
I feel so lucky to have worked with so many amazing people who worked tirelessly to save so many lives during the pandemic and I have never been prouder to work for the NHS.”
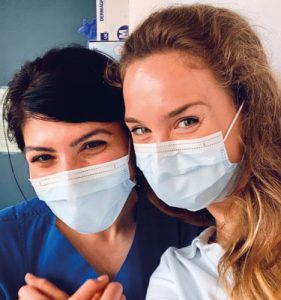 Elena Kasche (Queen’s 09)
Elena Kasche (Queen’s 09)
“Being a doctor in the largest teaching hospital in northern Germany, we quickly had to adapt to the situation. Overnight we switched from our daily routine with elective procedures to ‘emergencies only’ mode. The aim was to let the hospital run empty and to clear at least 40% of beds for incoming SARS-CoV-2 patients. Previously, we had been told not to wear any protective gear so we wouldn’t alarm the public. Although we later found out it was simply because we didn’t have enough for everybody.
Even after we were fully equipped, colleagues began to develop temperatures and test PCR-positive for the virus. That changed things up again. Half of us were working double shifts while the other half had to undergo involuntary quarantine for two weeks. Luckily, nobody became seriously ill. Teaching sessions, staff meetings and patient visits were suspended until further notice. Nobody could leave the country – let alone state.
Germany went into a moderate lockdown and hospitals went into major lockdown. Social distancing helped and, fortunately, we never reached full capacity, which allowed us to treat patients from Italy and Spain in our Intensive Care Unit. We are now preparing for a potential second wave that will hopefully never hit.
Our hospital has been made the SARS-CoV-2-Centre in northern Germany and while other hospitals are going back to some form of business as usual, we have to stand by and keep 25% of beds ready for incoming SARS-CoV-2 patients at all times. This puts an enormous strain on our health care system. Due to the lack of elective patients and inpatient beds, our department expects a huge dent in the budget despite all political efforts. As nobody knows what the future holds all we can do is remain calm and hopeful. Good luck to all of you and keep looking after each other.”
James Hill (Cobham 96)
“I founded Prescript Recruitment in Australia, we’re known for helping solve the regional doctor shortage. Australia is so big, with the population concentrated in coastal cities, that there is a considerable inequality with access to health care in rural and remote areas.
Covid-19 has been incredibly hard to navigate for our doctors and our clients – the different states and territories in Australia implemented their own border restrictions. This meant our team of Prescript doctors couldn’t travel interstate, putting massive pressure on regional areas that rely on locum doctors to keep their services running.
Each day we would wait, first for the Prime Minister to announce a new rule and then for each state leader to announce their variation. We all came to dread what the news would bring and how it would unpick all the carefully planned travel itinerary for doctors. The wobbles with our two leading airlines, Qantas and Virgin, worried us all too – Australia relies on planes for routine travel.
We’ve been so delighted by the response of our doctors and clients. For example, they have cheerfully signed up for Covid-19 fever clinics; they have quarantined happily for two weeks to be able to work in Tassie; plus, driven incredible distances to fulfil their commitment to a regional hospital. I am proud of Prescript’s role in making sure doctors are where they need to be!”
 Liz McEvoy (née Kerford-Byrnes, Stanhope 93)
Liz McEvoy (née Kerford-Byrnes, Stanhope 93)
“I am a GP in Rugby, Warwickshire, and during the Covid-19 pandemic I have seen my job change on a daily, and sometimes even hourly, basis until it has become completely unrecognisable from what I trained to do.
I now have remote contact with the vast majority of my patients, using telephone or, more recently, video calls to explore their symptoms and worries, diagnose and arrange treatment for them. A few make it in for a face-to-face appointment or get a home visit – there are certain things that simply can’t be done over the phone after all (cervical smear anyone?), but only after careful screening of symptoms and contacts that might indicate an active infection. But with around 80% of cases being asymptomatic, sometimes these precautions seem rather futile.
I also work sessions at the local ‘hot hub’ where confirmed or suspected Covid-19 cases are seen when a physical examination is deemed necessary. All these contacts are done wearing PPE, which in reality means wearing a flimsy plastic apron, a pair of gloves, a surgical mask and a homemade visor that makes me feel a bit like a Dalek! But it’s the best we have and our patients still need care for all the normal things alongside Covid-19, so we just cross our fingers and get on with it.
We’ve worked hard to keep the practice doors open despite self-isolation, shielding and pre-existing medical conditions decimating the clinical staff. We just hope we’re doing enough.”
Julian Barnbrook (Grafton 89)
“The hospital I work at in northern British Columbia (Canada) has probably had a very different experience to most of the UK. I work in Intensive Care Unit (ICU) and anaesthesia. Our physical distancing measures and restrictions on non-essential activities seem to have been pretty effective so far – we never had a full ‘lockdown’ as the UK did, but businesses other than groceries, pharmacies and take-aways were mostly closed and all non-urgent surgery was cancelled.
We never had the high degree of pressure on our resources that we had prepared for and – at present – our levels of infection are low and declining (all of which could change abruptly of course). I was part of a team responsible for airway management of possible Covid-19 patients (one of the more risky activities in terms of potential exposure), so I spent a fair amount of time performing procedures in full PPE (the head to toe covering etc).
We have had a total of five patients on our ICU, three who were critically ill and all have done well and been discharged home. This is probably one of the less dramatic Covid-19 accounts and there are certainly times when I felt a pang of guilt not to be with former colleagues in the thick of it in London.”
Neil Pottinger (Grafton 84)
“I am the Sales and Marketing Director for Starkey Hearing Technologies in the UK. Starkey is a global manufacturer of hearing technology and, in the UK, supplies both the private and public sector with hearing instruments.
During the pandemic those with untreated hearing challenges have had enormous issues in communicating with family and friends, whilst possibly also having to cope with self-isolation. A lack of ability to hear well is bound to have had an impact on people already dealing with the huge stresses presented by Covid-19. Loneliness and isolation can have a devastating impact on health and well-being.
Starkey have been able to continue to offer remote repair services and online support to clients, but we continue to try to do more through our audiology clients nationwide. Our hearing instruments incorporate fall detection and alerts, activity and social engagement tracking and, crucially in this period, a care app that allows family to check that their relatives are using their hearing instruments and getting some activity and conversations into their day. It is another layer of support that can help make all the difference.
We must also consider the financial impact on our customers and have worked hard to support them in getting back to business. We continue to provide guidance and support to those in the front line of providing audiology services.”
 John Buchanan (Chandos 82)
John Buchanan (Chandos 82)
“I work as a doubly qualified Oral Medicine Clinical Academic in a large teaching hospital in East London. Oral Medicine is a small dental specialty which involves the diagnosis and treatment of oromucosal conditions often with associated medical conditions.
The past three months have been particularly busy and the Covid-19 pandemic has had a real impact on East London. Early on in the pandemic, a rapid decision was made to close face-to-face outpatient care for all cases except emergencies. In addition to undertaking remote telephone consultations for Oral Medicine patients, I was also redeployed to support a medical service that looks after patients with a complex autoimmune disease treated with immunosuppressant agents.
Throughout this period I have been impressed by the dedication and teamwork shown by all of the staff involved in patient care both within the hospital and in the community. In common with many clinical academics involved in teaching, these past weeks have been particularly busy owing to the need to switch from face-to-face teaching to teaching and assessing in an online environment. I’ve noticed a significant improvement in my IT skills! We have a number of overseas students in the dental school who have returned to their home countries. It has been slightly awe-inspiring to realise that my lectures are being listened to by students in countries many thousands of miles away from London!
I have continued to commute into London travelling on eerily deserted trains and tubes, but have managed to work from home one day a week, which has allowed me to continue to be involved in educational research – some of which has a direct relevance to the Covid-19 pandemic.”
 Stuart Miller (Chatham 77)
Stuart Miller (Chatham 77)
“My working world as the Chief Medical Officer to the GB Paralympic Team was turned upside down at the beginning of March by the Covid-19 crisis. I was in Japan, sorting out some final arrangements for the 2020 Paralympic Games in a remarkably calm country, when British Airways highlighted our plight with a disturbing email ‘hoping’ rather than guaranteeing to get us back to the UK.
Soon after, all the sports centres closed – along with my clinic in the English Institute of Sport at the University of Bath, then the private hospital where I do a clinic was taken over by the NHS. In keeping with many health care workers, I volunteered to return to the ‘frontline’ but health issues have kept me away from what was a remarkably quiet NHS in our area of the South West.
Within all the sports that make up the Paralympic Games, we have about 100 shielded or vulnerable athletes who tried to keep up their fitness and preparation, but enthusiasm to maintain peak fitness is difficult when you hear that the Games have been postponed.
The slow return to the training environment has been perhaps the most challenging aspect of the crisis. Social distancing from a guide when you are a blind runner, clearly does not work; having to enlist the help of those around you in a gym environment or getting in and out of a boat increases risks. All sorts of other challenges that raise questions about safety in athletes with a disability tested our systems and required meticulous planning.
A huge amount of work has taken place to help guide the sports and their athletes back to the training environment, which has kept me tied to my home office whilst my wife Carly and daughter Kathryn battle with the challenges of the outside world as a GP and as a junior doctor. One has already had the virus but being young and healthy has sailed through it except that she can no longer taste chocolate! Some things are hard to bear!”
 Dr John Coleman, OBE (Chandos 58)
Dr John Coleman, OBE (Chandos 58)
“My experiences in lockdown have been challenging and creative, as well as being more rewarding than I could have expected.
As a psychologist with vast experience in work with parents and teenagers, I was encouraged to use some of my knowledge to provide advice and guidance. Using my contacts in charities that deal with family problems or with mental health issues, I began to write blogs and create podcasts to help parents and young people navigate through this unprecedented situation.
I have been so pleased that my work has been found to be useful. I have made a huge leap forward in my ability to use online meeting technology and I am now running workshops for parents, as well as for social workers and other professionals. In June, 100 parents attended my workshop on teenagers and brain development! I also ran another workshop for parents entitled ‘Don’t give up on your teenager: you are needed more than ever!’
I am fortunate that I have been able to put my knowledge to work. To be able to give something back has given me a purpose in this extraordinary lockdown space.”
THANK YOU on behalf of all Old Stoics to all NHS staff and key workers, you are doing incredible jobs and we can’t thank you enough. Your courage and compassion will be remembered for many years to come.

